Psoriatic arthritis is a chronic inflammatory form of arthritis associated with the skin condition psoriasis. Up to 30% of people with psoriasis can develop psoriatic arthritis. This autoimmune condition causes joint pain, swelling and stiffness and can also affect the skin, nails and other organs. As a rheumatology expert, I’ve written this detailed guide to psoriatic arthritis covering the causes, symptoms, diagnosis process and latest treatments available.
What Causes Psoriatic Arthritis?
The exact trigger for psoriatic arthritis is unknown, but it is believed to have both genetic and immune system components:
- Genetics – Having genes linked to psoriasis and HLA-B27 antigen increases risk. About 40% of patients have a family history.
- Immune system – A mistaken attack by the immune system causes inflammation in joints and skin.
- Environmental factors – Viral or bacterial infections may trigger this condition in genetically predisposed people. Physical trauma, certain medications and stress can also contribute.
While the mechanisms are not fully clear, white blood cells cause uncontrolled inflammation in the joints, skin and connective tissue of patients.
Symptoms of Psoriatic Arthritis: People With Psoriasis Experience Chronic Inflammation

Photo Credit: tommyandone, Envato
Psoriatic arthritis causes a variety of symptoms that can appear separately or together:
Joint Symptoms
- Joint pain, swelling and tenderness, especially in the knees, fingers and toes.
- Reduced range of motion and stiffness in the affected joints.
- A symmetrical pattern of arthritis, meaning it affects the same joint on both sides.
- Joint deformities can develop in severe cases.
Skin Symptoms
- Patches of red, scaly skin or silvery plaques from psoriasis
- Nail changes like pitting, ridges or discolouration
- Swelling and pain where tendons and ligaments attach to bone.
Other Symptoms
- Fatigue
- Low-grade fever
- Eye problems like conjunctivitis
Symptoms range from mild to severe. Some people with psoriatic arthritis may have skin symptoms before joint symptoms or vice versa. The disease course is unpredictable.
Types of Psoriatic Arthritis
There are different patterns in which psoriatic arthritis can develop:
- Asymmetrical oligoarticular – Affects four or fewer joints, typically in the fingers and toes, not the same on both sides. Most common type.
- Symmetrical polyarticular – Mimics rheumatoid arthritis. Affects five or more joints symmetrically on both sides of the body.
- Distal interphalangeal predominant – Affects last joints in fingers and toes.
- Arthritis mutilans – Rare and severe form that destroys small joints in hands and feet.
- Spondylitis – Inflammation of the spine causing stiffness and pain.
Who Gets Psoriatic Arthritis?
These factors increase the risk of developing psoriatic arthritis:
- Having psoriasis – Up to 30% of psoriasis patients develop this condition.
- Family history of psoriasis or psoriatic arthritis.
- Testing positive for the HLA-B27 gene.
- Having nail changes like pitting or ridges.
- Prior joint injury triggering this ailment.
- Being overweight – Excess weight puts mechanical stress on joints.
Psoriatic arthritis equally affects men and women. Onset is most common between ages 30 – 50 years old.
How is Psoriatic Arthritis Diagnosed?

Photo Credit: tommyandone, Envato
There is no single test for psoriatic arthritis. A rheumatologist diagnoses it based on:
- Patient history – Details about joint symptoms, psoriasis, and family history of arthritis.
- Physical exam – Evaluating joints for inflammation and range of motion. Checking skin and nails for psoriasis signs.
- Imaging tests – X-rays, MRI and ultrasounds check for joint damage.
- Blood tests – For markers of inflammation like ESR and CRP. Tests for rheumatoid factor and uric acid.
- Removing and testing joint fluid – Looking for inflammation.
Early diagnosis is important to prevent permanent joint damage from untreated inflammation. Tell your doctor about any suspicious symptoms.
How is Psoriatic Arthritis Treated? Goals, Approaches & Treatment for Psoriatic Arthritis
The goals for psoriatic arthritis treatment are:
- Relieve pain and inflammation
- Slow or prevent joint damage
- Improve ability to perform daily activities
- Minimize functional disability
This typically involves medications, lifestyle changes, occupational therapy, and sometimes surgery.
Medications
- NSAIDs – Relieve pain and inflammation. Naproxen and ibuprofen are commonly used.
- DMARDs – Disease-modifying antirheumatic drugs like methotrexate, and sulfasalazine suppress the overactive immune system response.
- Biologics – Target specific parts of the immune system. Examples are etanercept, adalimumab, and infliximab.
- Corticosteroids – Potent anti-inflammatory drugs like prednisone. Given through pills, injections or topically.
- TNF inhibitors – Block the TNF cytokine involved in inflammation. Very effective for this ailment.
Lifestyle Measures and Home Remedies
- Apply warm and cold compresses to relieve joint pain.
- Perform low-impact exercises like swimming regularly to improve joint mobility.
- Use joint protection techniques like bracing and assistive devices to prevent injury.
- Reduce stress through relaxation techniques, meditation, yoga, and tai chi.
- Maintain a healthy diet and body weight. Omega-3 fatty acids help reduce inflammation.
- Quit smoking, as tobacco use worsens symptoms.
- Supplements like turmeric, ginger, and Boswellia may help reduce inflammation and pain.
Physical and Occupational Therapy
- Stretching, strengthening and aerobic exercises improve function.
- Modalities like heat, ice, and TENS help relieve pain.
- Joint mobilization techniques provide pain relief.
- Assistive devices like canes, walkers, and orthotics support mobility.
Surgery
- Joint replacement surgery in cases of severe joint damage and disability.
- Surgery to repair tendons or correct joint deformities.
- Spinal fusion surgery if the spine is severely affected.
Self-care Tips and Living with Psoriatic Arthritis

Photo Credit: tommyandone, Envato
- Get regular exercise to improve strength, flexibility and cardiovascular fitness. Try swimming, cycling and walking.
- Use joint protection strategies – avoid lifting heavy objects, don’t overuse sore joints, and use assistive devices.
- Apply hot packs or take warm baths before activity, and ice packs after activity to relieve sore joints.
- Maintain a healthy diet and weight to avoid extra stress on weight-bearing joints.
- Reduce stress through relaxation techniques, counselling or joining a support group.
- Take medications as prescribed and keep up with medical appointments.
- Listen to your body – rest joints when in pain or fatigued.
- Use ergonomic tools and make home modifications like installing grab bars to ease daily tasks.
- Avoid repetitive, high-impact activities that can damage joints.
While living with psoriatic arthritis poses challenges, being proactive with treatment and self-care allows maintaining an active, fulfilling life. Reach out to your doctor and support system if symptoms worsen or mobility declines. Research continues to provide hope for less painful, disability-free lives for patients.
Potential Complications of Psoriatic Arthritis
If left untreated, this chronic condition can worsen over time and cause permanent joint damage or disability. Potential complications include:
- Severe joint deformity causing loss of hand and finger function
- Spinal flexion issues from fused vertebrae. Can compress spinal nerves.
- Osteoporosis and increased fracture risk from inactivity and medications
- Joint damage requiring eventual joint replacement surgery
- Atherosclerosis and higher incidence of cardiovascular disease
- Eye inflammation disorders like uveitis and conjunctivitis
- Liver toxicity from certain medications like methotrexate
- Depression and social isolation from chronic joint pain and disability
Early diagnosis and appropriate treatment helps prevent or delay these complications and improves overall prognosis and quality of life.
Research and Emerging Psoriatic Arthritis Treatment
Research continues to better understand the inflammatory form and discover improved treatments targeting the inflammatory process driving this condition.
Current Research Directions
- Identifying genes and immune pathways involved in psoriatic arthritis
- Developing targeted biologic drugs that block specific parts of the inflammatory process
- Using stem cell therapy to repair damaged joint cartilage
- Studying the impact of the gut microbiome on psoriatic arthritis
Emerging Treatments
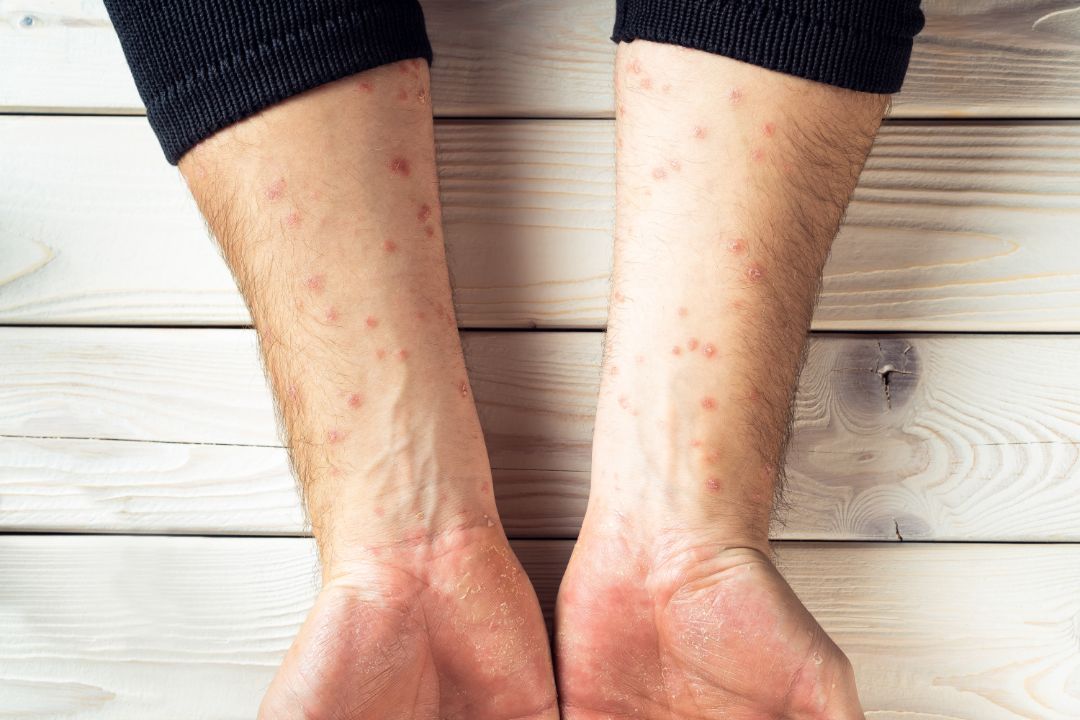
Photo Credit: jeannierv, Envato
- New biologic agents like interleukin (IL) inhibitors that target cytokines driving inflammation
- Small molecule drugs like JAK inhibitors and PDE4 inhibitors that regulate immune cell activity
- Biosimilar versions of current biologic drugs to improve affordability and access
- Targeted synthetic DMARDs like apremilast with fewer side effects
The future looks brighter for patients. With increased knowledge of the disease mechanisms and advanced treatment options to halt the inflammatory process, better management of this chronic condition is on the horizon.
Frequently Asked Questions About Psoriatic Arthritis
What are the early warning signs of psoriatic arthritis?
Early signs of psoriatic arthritis include joint pain and swelling, morning stiffness, reduced range of motion, and nail changes like pitting or ridges in those with psoriasis.
Where does psoriatic arthritis usually start?
Psoriatic arthritis often first appears in the joints of the fingers, toes, knees, ankles and wrists, though it can start in any joint.
What is the main cause of psoriatic arthritis?
The exact cause is unknown but it’s believed to be an immune system dysfunction causing inflammation in joints and skin in genetically predisposed individuals.
What virus causes psoriatic arthritis?
No virus is known to directly cause psoriatic arthritis, though viral infections may trigger the onset of psoriatic arthritis in those with a genetic predisposition. More research is needed.



