Lupus is an autoimmune disease where the immune system attacks its own healthy cells and tissues. This arthritis results in inflammation and damage to various parts of the body. Lupus is also known as systemic lupus erythematosus (SLE). Here is an in-depth look at the causes, symptoms, diagnosis and treatment options for lupus.
Causes of Lupus

Photo Credit: varyapigu, Envato
The exact causes of lupus are unknown. Research suggests that a combination of genetic, environmental and hormonal factors may trigger lupus in susceptible individuals.
Genetic Factors
People with a family history of lupus or other autoimmune disorders are at a higher risk of developing lupus. The presence of certain genes makes the immune system prone to overactivity and self-attack.
Environmental Triggers
Exposure to certain medications, chemicals, viruses or UV light may initiate lupus in those with genetic susceptibility. Some potential triggers include:
- Medications: Hydralazine, procainamide, isoniazid, chlorpromazine
- Viruses: Epstein-Barr virus, cytomegalovirus
- UV light and Sun Exposure
- Chemicals: Silica, aromatic hydrocarbons
Hormonal Influences
- Women are 9 times more likely to develop lupus. Estrogen can stimulate the immune system and exacerbate lupus.
- Fluctuating estrogen levels during pregnancy can cause lupus relapses and flares.
- Lupus onset or flares are also common during puberty, childbirth and menopause.
Symptoms of Lupus
Lupus affects people differently. Symptoms may come and go over time. The most common symptoms are:
Fatigue and Fever
- Extreme fatigue and tiredness
- Unexplained fever over 100°F
Skin Problems
- Butterfly facial rash over the cheeks and bridge of the nose
- Rashes on the arms, legs and torso
- Photosensitivity – skin rashes worsen with sun exposure
- Fingers turn white or blue in the cold (Raynaud’s)
Joint Pain
- Pain, swelling and stiffness in joints
- The most commonly affected joints are the hands, wrists, elbows, knees, ankles
Chest Pain
- Sharp chest pain when taking a deep breath
- Chest pain due to inflammation of the lung lining (pleurisy)
Other Symptoms
- Headache, confusion and memory loss
- Mouth or nose ulcers
- Hair loss
- Fingers turning white or blue when cold (Raynaud’s phenomenon)
Diagnosing Lupus
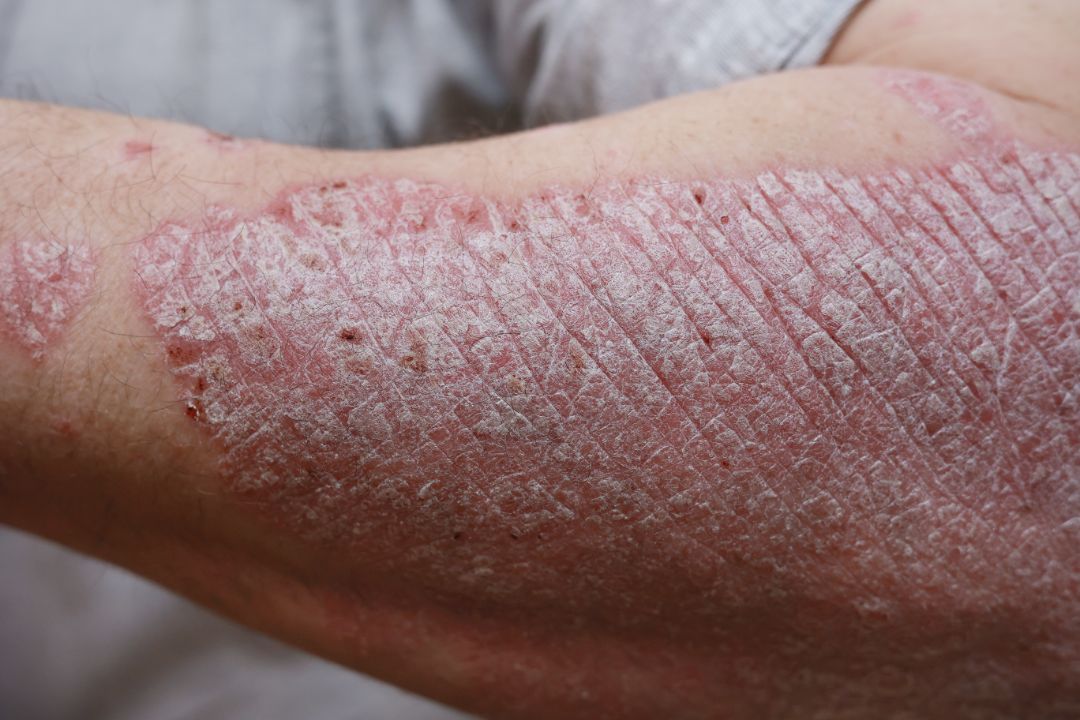
Photo Credit: andriymedvediuk, Envato
There is no single test to diagnose lupus. Doctors will analyze symptoms, conduct a physical exam and run laboratory tests to rule out other conditions. Common diagnostic tests for lupus include:
Blood Tests
- Complete blood count to check for anemia, low blood platelets and white blood cells
- ESR for inflammation
- CRP for inflammation
- Antinuclear antibody (ANA) test – positive in 95% of lupus patients
- Anti-dsDNA, anti-Ro/SSA, anti-LA/SSB – positive in 60-70% of lupus patients
- Complement levels – C3 and C4 may be low indicating lupus activity
- Kidney and liver function tests
Urine Tests
- 24-hour urine protein – excessive protein indicates kidney involvement
- Urine protein/creatinine ratio
Imaging Tests
- X-rays of joints and chest to detect inflammation and damage
- Echocardiogram to examine heart function
Skin Biopsy
- Taking a small skin sample to check for inflammation and vasculitis
Lupus Treatment Approach
While there is no cure yet for lupus, treatments focus on managing symptoms and preventing flares. A combination of self-care, medications and lifestyle changes helps control lupus.
Medications
Common medications used are:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – for pain relief and inflammation
- Antimalarials like hydroxychloroquine – prevent flares and organ damage
- Corticosteroids – prednisone to quickly reduce inflammation and pain
- Immunosuppressants – azathioprine, mycophenolate to restrain the overactive immune system
- Biologic drugs – belimumab targets B cells to reduce antibodies
Lifestyle Changes
- Avoid sun exposure and use sunscreen – prevents rashes and flares
- Get enough rest and sleep – reduces fatigue
- Follow an anti-inflammatory diet – with omega-3s and antioxidants
- Reduce stress – meditation, yoga and counseling help
- Quit smoking – to minimize cardiovascular risks
- Exercise regularly – low-impact activities like walking, swimming
Self-care and Supportive Care
- Use moisturizers and topical creams – reduces skin irritation
- Take calcium and vitamin D supplements – for bone health
- Be aware of infections – due to weakened immunity
- Join a support group – for coping with the emotional aspects of lupus
Close monitoring and follow-up care by a rheumatologist is essential to keep lupus symptoms under control. Seek prompt medical attention if you notice worsening joint pain, rashes, chest pain or breathing difficulties that could indicate a disease flare or complication. The treatment goal is to improve quality of life and prevent organ damage from complications of uncontrolled lupus activity. Here is a continuation of the lupus article:
Complications of Lupus
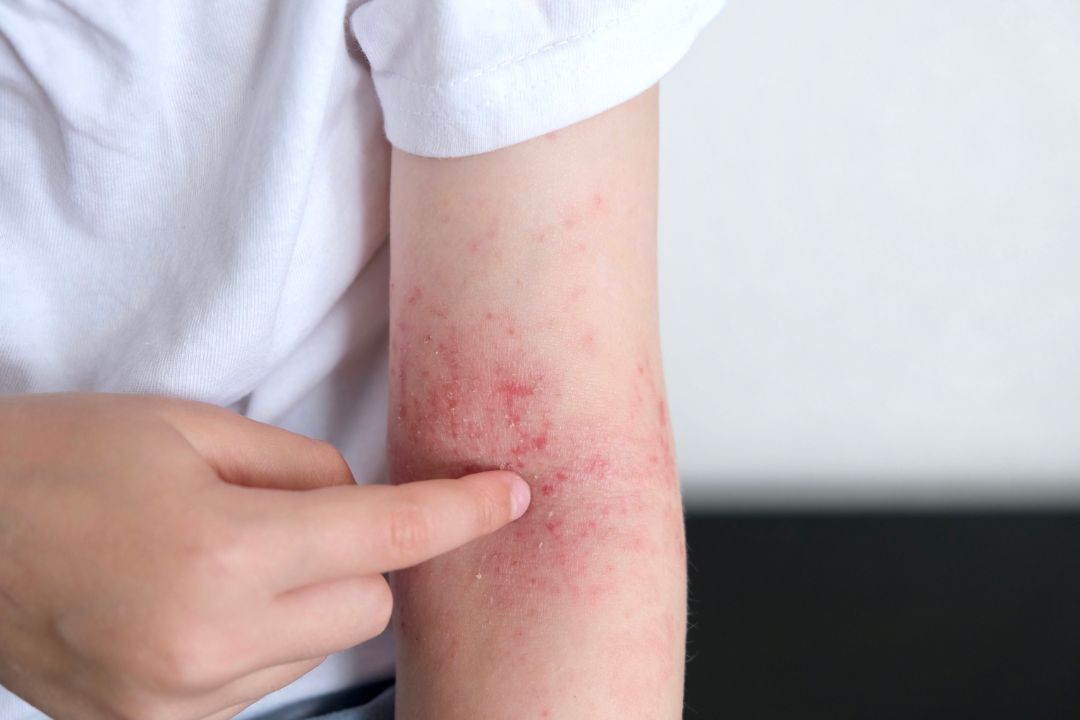
Photo Credit: MarishkaTR, Envato
When lupus is active and uncontrolled, it can affect multiple organs and cause serious complications:
Lupus Nephritis
- Inflammation of the kidneys occurs in 50% of lupus patients
- Causes blood and protein in the urine, swelling in the legs and high blood pressure
- Requires urgent treatment with corticosteroids, immunosuppressants
- This may lead to permanent kidney damage and kidney failure
Cardiovascular Disease
- Accelerated atherosclerosis causes an increased risk of heart attacks and strokes
- Inflammation can cause damage to heart valves (endocarditis)
- Pericarditis can occur with inflammation of the sac around the heart
Lung Complications
- Inflammation of lung tissue (pleuritis) causes chest pain
- Higher risk of bronchitis, pneumonia and pneumonitis
- May cause scarring and shrinkage of lung tissue
Blood Disorders
- Anemia due to red blood cell destruction and inflammation
- Leukopenia or low white blood cells due to an immune cell attack
- Increased risk of infections and sepsis
Pregnancy Complications
- Increased frequency of miscarriage, preeclampsia, preterm birth
- Chance of neonatal lupus in a baby with anti-Ro/SSA antibodies
- Postpartum flares are common due to shifting hormone levels
Living with Lupus
Coping with a chronic illness like lupus can be challenging. Some tips that help:
- Learn about your condition and be involved in treatment decisions
- Notice and avoid triggers that worsen your symptoms
- Maintain a healthy and active lifestyle with exercise and nutrition
- Protect yourself from stress, fatigue and infections
- Join a local or online support group to share experiences
- Communicate with family and friends for emotional support
- Seek counselling or therapy if dealing with depression or anxiety
Lupus research is ongoing to understand better what causes it and to discover more targeted treatments. While there is currently no cure, with the right treatment plan lupus symptoms can be managed effectively over the long term.
Frequently Asked Questions About Lupus
What is the life expectancy of a person with lupus?
The life expectancy for lupus patients today is close to normal unless critical organs like the heart and kidneys are severely affected. Most people with lupus can expect to live a normal lifespan with treatment.
How serious is lupus disease?
Lupus is an autoimmune disease that, if untreated, can damage critical organs and be life-threatening. With proper treatment, symptoms can be managed and organ damage avoided, making lupus a serious but manageable disease.
Why does a person get lupus?
The exact cause is unknown, but genetic, hormonal and environmental factors trigger lupus in those predisposed to it. Immune system dysfunction leads to inflammation and damage.
What are the four signs of lupus?
The four common signs of lupus are fatigue, joint pain or swelling, skin rashes, and fever of 100°F or higher that other causes cannot explain.


