If you’ve experienced shoulder pain or instability, you know how frustrating and debilitating it can be. Shoulder instability is a common problem affecting people of all ages and backgrounds.
It occurs when the ball of the upper arm bone moves out of its socket, causing pain and discomfort.

Photo Credit: JoPanwatD, envato
If you’re experiencing shoulder pain or discomfort, it’s essential to determine whether shoulder instability might be to blame. Here are some of the most common symptoms:
These symptoms can be an indication of shoulder instability, and anyone experiencing them should seek medical attention to determine the underlying cause.
Shoulder instability can occur due to a variety of reasons. Understanding the underlying causes can help individuals take preventative measures to reduce their risk of developing the condition.
A previous injury is one of the most common causes of shoulder instability. This includes dislocations, subluxations, and rotator cuff tears. When the shoulder joint has been injured, it becomes more susceptible to future instability as the ligaments and muscles around it may weaken.
Individuals who frequently engage in repetitive overhead motions, such as athletes who play overhead sports or construction workers who use jackhammers, may be at an increased risk of developing shoulder instability. These motions can cause wear and tear on the shoulder joint, leading to instability over time.
If the ligaments or muscles in the shoulder are weak, they may be unable to properly support the joint, leading to instability. This can be caused by genetics, inactivity, or other medical conditions.
Some individuals may be genetically predisposed to shoulder instability. This is often due to inherited conditions that affect the structure or stability of the shoulder joint, such as Ehlers-Danlos syndrome.
By understanding the potential causes of shoulder instability, individuals can take proactive measures to reduce their risk of developing the condition. This may include avoiding repetitive overhead motions, participating in regular exercise and strength training, and seeking treatment for any previous shoulder injuries.
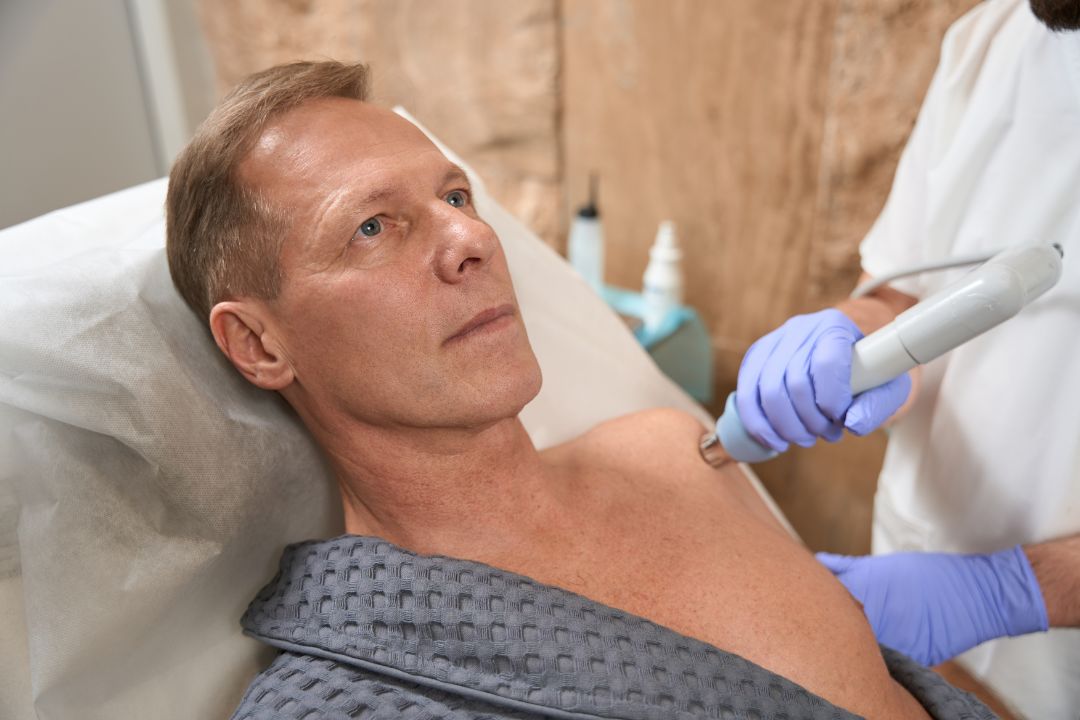
Photo Credit: svitlanah, Envato
Treatment for shoulder instability can range from non-surgical options to complex surgery. The right course of treatment will depend on the severity of the instability and the underlying cause.
Physical therapy exercises are often the first line of treatment for shoulder instability. Specific exercises can be prescribed to strengthen the muscles and ligaments around the shoulder joint, which can help improve stability.
A physical therapist may also use ultrasound or electrical stimulation techniques to help reduce pain and inflammation.
Working closely with a qualified physical therapist is important to ensure proper technique and avoid further injury.
If non-surgical options aren’t effective, surgery may be necessary to stabilize the shoulder. The exact surgical approach will depend on the patient’s individual situation, but common options include:
The surgeon will determine the surgical approach based on the patient’s specific needs and goals.
After surgery, rehabilitation is a critical part of the recovery process. A physical therapist will work with the patient to develop a rehabilitation plan that includes exercises to restore strength and range of motion in the shoulder.
 Photo Credit: svitlanah, Envato
Photo Credit: svitlanah, Envato
The rehabilitation process can be lengthy and may take several months to a year to fully recover. However, with proper care and rehabilitation, most patients can expect to return to their normal daily activities and even athletic pursuits.
If you’re experiencing symptoms of shoulder instability, you likely have many questions about the condition. Here, we’ll provide answers to some frequently asked questions to help you better understand the condition and how to manage it.
There are several things you can do to help prevent shoulder instability. One of the most important is to avoid repetitive overhead motions, which can put a lot of strain on the shoulder joint. Strengthening the muscles around your shoulder is also a good idea, as this can help improve stability. If you’ve had a previous shoulder injury or surgery, following your doctor’s instructions for rehabilitation and recovery is important to help prevent future problems.
In some cases, shoulder instability can be treated without surgery. Physical therapy exercises can help strengthen the muscles around the shoulder, which can improve stability. If you have mild symptoms of shoulder instability, your doctor may recommend a period of rest and immobilisation to allow the joint to heal. However, surgery may be necessary to repair the damage and improve stability if you have severe symptoms or frequent dislocations.
Rehabilitation after shoulder instability surgery typically involves several weeks of immobilisation, followed by several months of physical therapy. During the immobilisation period, you’ll wear a sling to help keep your shoulder stable as it heals. Once the sling is removed, you’ll work with a physical therapist to help improve range of motion and strengthen the muscles around the shoulder joint. It’s important to follow your doctor’s instructions for rehabilitation closely to ensure the best possible outcome.
In most cases, patients are able to return to their normal activities after shoulder instability surgery. However, following your doctor’s instructions for rehabilitation and recovery closely is important to ensure the best possible outcome. Depending on the nature of your injury and the type of surgery you had, you may need to modify certain activities or avoid certain movements to help prevent future problems.
The long-term outlook for shoulder instability depends on a variety of factors, including the severity of your injury, the type of treatment you receive, and how well you follow your doctor’s instructions for rehabilitation and recovery. In general, most patients are able to recover fully from shoulder instability with proper treatment and rehabilitation. However, some patients may experience ongoing symptoms or may be at risk for future dislocations. Your doctor can help you develop a plan to manage your symptoms and reduce your risk of future problems.