Heel spurs are bony protrusions that develop on the bottom of the heel bone due to repetitive stress and strain on the foot. They often occur with conditions such as plantar fasciitis, which involves inflammation of the thick tissue band running across the bottom of the foot.
What is a Heel Spur?
A heel spur is an abnormal calcium deposit or bony protrusion that develops on the bottom of the heel bone (calcaneus).
- Also called a calcaneal spur
- Often associated with plantar fasciitis
- Caused by repeated stretching of the plantar fascia ligament and flexor digitorum brevis muscle on the heel bone
- Pain and inflammation at the spur site
- Diagnosed via x-ray, MRI or ultrasound imaging
- Treatments include rest, orthotics, physical therapy, medications, shockwave therapy, heel spur surgery
Understanding the causes and risk factors for heel spurs allows prevention.
Heel Spur Symptoms

Photo Credit: fabrikasimf
The typical symptoms associated with heel spurs include:
- Pain under the heel or in the arch, especially with first steps in the morning or after rest
- Pain that gradually increases over time
- Swelling, redness or bruising under the heel
- Tightness or limited mobility in the foot and ankle
- Heel pain that is relieved by rest
- Irritation of the plantar fascia ligament
- Limping or altered gait from foot discomfort
- Sharp pain when pressing on the spur location
Seek evaluation for worsening or chronic heel pain, as it may signify a heel spur.
What is the Cause of Heel Spurs?
Common causes of heel spurs include:
- Plantar fasciitis – Repeated microtears and tension on the plantar fascia pulls on its attachment at the calcaneus leading to bone spur formation.
- Tight calf muscles – Short, stiff calf muscles increase strain and pull on the plantar fascia.
- Foot mechanics issues – High foot arches, overpronation, excessive foot rotation.
- Poor shoes – This condition can also develop from wearing shoes that lack of arch support and shock absorption. High heels.
- Obesity – Excess weight puts more stress on the feet.
- Aging – Plantar fascia loses elasticity and shock absorption over time.
- Diabetes – Peripheral neuropathy causes reduced sensation and tissue damage.
- Foot trauma – Fractures, injuries damaging the heel area.
- Running/jumping sports – High impact forces on the heel.
Activities involving heavy pressure onto the heels contribute to spur development.
Risk Factors for Heel Spurs

Photo Credit: yanalya
Factors that increase risk of getting heel spurs:
- Plantar fasciitis
- Tight calves, limited ankle flexibility
- High foot arches
- Overpronation or excessive inward foot rolling
- Occupations involving long periods on feet
- Regular running or high impact exercise
- Obesity
- Poor footwear with inadequate arch support
- Diabetes
- Older age
- Prior foot injuries
Evaluating personal risk factors allows proactive prevention.
Diagnosing Heel Spurs
Heel spurs are diagnosed through:
- Medical history – Foot symptoms, chronic plantar fasciitis history, and ailments in the foot that always cause pain
- Physical exam – Tenderness when pressing along plantar fascia, passive ankle range of motion
- Imaging – X-rays, MRI or ultrasound confirm bony heel spur
- Podiatrist evaluation – For specialized foot assessment
Tell your doctor about any prior heel pain, injuries or foot abnormalities. Both heels may be evaluated to compare.
Heel Spur Treatment Approaches – Treating Heel Spurs with Home and Medical Approaches
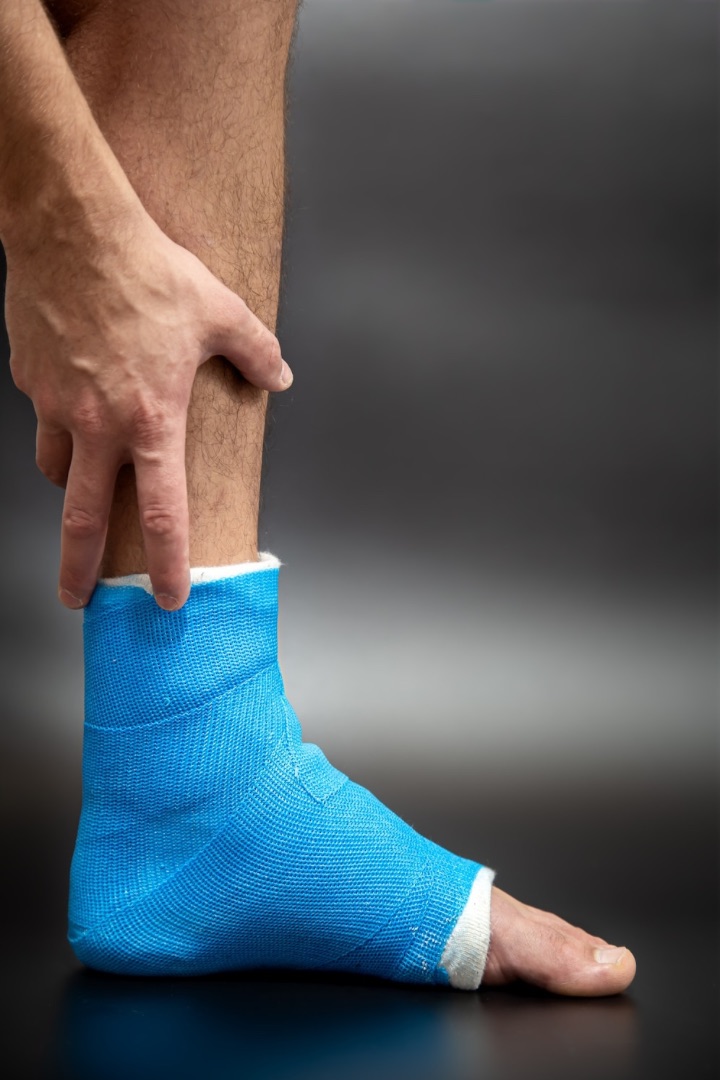
Photo Credit: pvproductions
Initial treatment options for heel spur pain aim to relieve inflammation, alleviate pain and remove pressure off the affected area:
Home Care
- Rest – Avoid prolonged standing/walking that aggravates pain.
- Ice – Apply ice packs to heel for 15 minutes daily to reduce swelling.
- Pain medications – Anti-inflammatories like Advil or Aleve can alleviate symptoms.
- Stretching – Gently stretch calves and plantar fascia once initial pain improves.
Medical Treatments
- Orthotics – Custom orthotic inserts support the arch to offload the spur.
- Night splint – Keeps the plantar fascia and Achilles tendon stretched overnight.
- Physical therapy – Stretching, massage, exercises improve mobility.
- Steroid injections – Powerful anti-inflammatories injected into the heel.
- Shockwave therapy – Pulses stimulate healing responses and reduce inflammation.
- Surgery – Endoscopic or open spur removal for severe refractory cases.
Conservative treatments are effective for to relieve heel spurs in most cases. Patients with diabetes or circulatory issues may need urgent care. Surgery to remove heel spurs is the last resort of treatment.
How to Prevent Heel Spurs? Prevention and Self-Care Tips
Methods to help prevent heel spurs include:
- Stretching the plantar fascia and calves multiple times daily
- Wearing supportive, well-fitted shoes with shock absorption and arch support
- Using orthotic shoe inserts recommended by a podiatrist
- Applying ice after exercise to minimize plantar fascia inflammation
- Losing excess weight to avoid overloading the feet
- Limiting extended standing and high impact activities
- Warming up before exercise and gradually ramping up activity
- Maintaining proper foot alignment and mechanics
Being proactive helps avoid heel pain and spurs. See a podiatrist for footwear recommendations and orthotics if needed.
Long-Term Outlook for Heel Spurs and Heel Pain
Most heel spurs and heel pain resolve in 6-12 months with appropriate traditional treatments, though symptoms wax and wane. Underlying mechanical causes like overpronation may need correction to prevent recurrence. Recovery can take longer for those with diabetes or circulation issues.

Photo Credit: fabrikasimf
Rarely, in debilitating circumstances a doctor may recommend surgery if all other treatments fail. Post-surgery, using braces and continuing calf/foot stretches and exercises helps prevent the heel spur and pain from returning. Activity modification, icing after exercise, and supportive footwear also keep symptoms at bay long-term.
FAQs
How do I get rid of a spur in my heel?
Heel spurs are often treated with rest, icing, braces, physical therapy stretching and exercises, anti-inflammatory medications, and sometimes steroid injections or shockwave therapy. In rare severe cases surgery may be required if heel spurs don’t respond to conservative treatments.
How do I know if it’s a heel spur?
Signs it may be a heel spur and not just plantar fasciitis include chronic, worsening heel pain that persists even at rest, pain upon standing after long periods of sitting, and heel tenderness localized to the spur site. Diagnostic imaging like x-ray or MRI can confirm.
How do I know if I have plantar fasciitis or heel spurs?
Plantar fasciitis causes diffuse pain along the arch and heel that worsens with activity. Heel spurs may cause pain where the spur is located, especially after rest. Heel spurs often accompany chronic plantar fasciitis.
Is walking OK for heel spur?
Walking is generally ok for heel spurs, even beneficial, as long as it does not significantly worsen pain. Use supportive shoes, orthotics, and ice after walking to prevent inflammation. Avoid extended walking periods.



