Vestibular physiotherapy, a specialised treatment modality, addresses symptoms provoked by vestibular system disorders.
The vestibular system within the inner ear is critical in maintaining balance and spatial orientation. When disrupted, individuals may experience debilitating symptoms such as dizziness, vertigo, and balance issues.
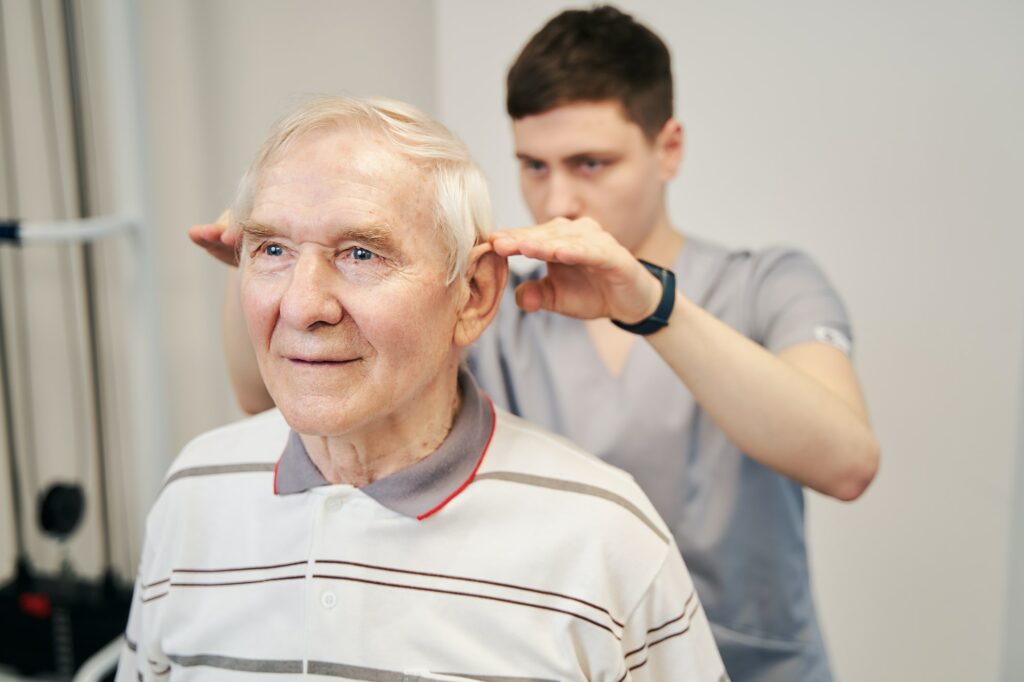
Through targeted techniques, including balance training, therapeutic exercises, and manual therapy underpinned by patient education, vestibular physiotherapy aims to alleviate these symptoms. This form of treatment is particularly beneficial for patients with conditions such as Ménière’s disease or benign paroxysmal positional vertigo (BPPV) and those rehabilitating from strokes or brain injuries.
Utilising bespoke treatment plans designed to enhance balance, coordination, and eye movements while reducing dizziness and vertigo through stimulation of the vestibular system, it offers an innovative approach towards improving quality of life.
Efficacy hinges on individual commitment to prescribed physical exercises and lifestyle modifications.
Vestibular physiotherapy, a specialised form of treatment, targets the alleviation of symptoms such as dizziness, balance issues, and problems with spatial orientation brought about by disorders affecting the vestibular system located within the inner ear.
This therapeutic approach utilizes various techniques incorporating vestibular rehabilitation exercises designed to stimulate and retrain the compromised vestibular system. These exercises aim to improve balance, coordination and eye movements, thereby significantly reducing vertigo or dizziness associated with vestibular disorders.
A comprehensive vestibular assessment is integral in tailoring an individualised treatment plan that caters to specific needs. Early intervention through this non-invasive method has been shown to mitigate the long-term impacts of these conditions, fostering innovative solutions towards improved quality of life.
Symptoms such as dizziness, vertigo, and balance difficulties often indicate disorders of the inner ear’s crucial system for maintaining equilibrium and spatial orientation. These disruptions can be due to central vestibular dysfunction or peripheral ailments like benign paroxysmal positional vertigo (BPPV).

BPPV is characterised by a false sensation of spinning, often triggered by specific changes in head position. Furthermore, balance disorders may manifest through instability during locomotion or standing still. Vestibulo-ocular reflex (VOR) abnormalities might lead to issues with eye movements and vision stability during head motion.
Innovative interventions like vestibular physiotherapy provide vertigo therapy to modulate these symptoms through tailored exercises designed to retrain the VOR and improve overall balance control.
Beneficial techniques employed in this specialised therapy area encompass balance training, specific exercises, manual therapy, and education about the condition, each tailored to an individual’s unique needs and symptoms.
Balance exercises are crucial for enhancing postural stability and reducing dizziness. Techniques such as canalith repositioning maneuvers can alleviate vertigo by repositioning dislodged otoliths in the inner ear.
Gaze stabilisation exercises improve visual focus during head movement, assisting with spatial orientation. Proprioceptive exercises enhance body awareness in space while improving equilibrium. Postural stability training further reinforces balance and prevents falls.
The amalgamation of these evidence-based strategies within vestibular physiotherapy offers an innovative approach that significantly advances treatment outcomes for individuals suffering from vestibular disorders.
Tailored treatment plans, meticulously crafted by expert physiotherapists to meet each patient’s unique needs and symptomatology, have shown remarkable efficacy in managing disorders of the inner ear balance system.
Employing a multi-faceted approach rooted in evidence-based practice, vestibular physiotherapists utilise targeted techniques such as balance retraining and sensory integration therapy. These personalised interventions not only address existing symptoms but also mitigate future complications.

Tailored treatment plans incorporating neurological physiotherapy principles focus on improving nerve function and overall neural health. This innovative therapeutic strategy fosters an integrated approach towards recovery, ensuring comprehensive care for individuals affected by vestibular disorders.
Thus, a commitment to individualised treatment planning forms the backbone of effective vestibular physiotherapy intervention.
Integral to the success of treatment for inner ear balance disorders is the role played by the trained physiotherapist. In vestibular physiotherapy, they employ tailored techniques such as head movement exercises and balance retraining, designed to stimulate and re-educate the vestibular system.
The physiotherapist’s role extends beyond direct intervention; they also take charge of fall prevention, coaching patients on safe mobility strategies to mitigate risks associated with dizziness and imbalance. Furthermore, they address visual-vestibular interaction concerns by prescribing exercises that help improve gaze stability.
Thus, through the expert application of evidence-based interventions and patient education, physiotherapists play an indispensable role in improving outcomes for individuals undergoing vestibular rehabilitation.
The choice between home-based and clinic-based therapy for balance disorders is a critical decision that can significantly impact an individual’s recovery journey. Both settings have unique merits in treating vestibular hypofunction or cervicogenic dizziness.
Home-based therapy allows for more flexible scheduling and comfort, facilitating compliance with the prescribed regimens for managing motion sensitivity and dizziness treatment.

Conversely, clinic-based therapy provides immediate access to trained professionals who can adjust interventions as needed, particularly beneficial in managing complex conditions such as vestibular migraine.
It is paramount that the chosen environment fosters adherence to the therapeutic regime while ensuring safety during activities aimed at retraining the vestibular system. The ultimate goal remains improvement in function and quality of life.
Successful rehabilitation outcomes hinge on a patient’s dedication and adherence to the prescribed therapeutic regimen, underscoring the importance of commitment in managing balance disorders. The efficacy of vestibular physiotherapy is highly contingent upon patient engagement, particularly in conditions like Ménière’s disease, labyrinthitis, and other inner ear disorders.

Adherence to prescribed exercises fosters neuronal plasticity within the vestibular system – a vital aspect of recovery from these conditions. Regularly performing these exercises not only alleviates symptoms but also aids in preventing relapses.
Thus, commitment to treatment extends beyond immediate symptom management; it underpins long-term functional restoration and quality-of-life improvement. Therefore, fostering patient commitment towards vestibular physiotherapy is integral to successful treatment outcomes for balance impairments due to vestibular disorders.
Empirical evidence underscores the efficacy of this therapeutic approach in managing balance disorders and improving quality of life. In many scientific studies, vestibular physiotherapy has demonstrated significant potential in alleviating symptoms associated with vestibular disorders.
This non-invasive treatment option utilises dynamic exercises and targeted lifestyle modifications to stimulate and retrain the vestibular system. Consequently, it fosters enhanced coordination, spatial orientation, and balance proficiency, fostering improved overall well-being.
The individualised nature of the therapy permits tailored interventions that address specific patient needs. While the success rate largely hinges on commitment to the treatment regimen, early intervention can substantially mitigate the long-term impacts of vestibular disorders.
Therefore, innovative healthcare solutions like vestibular physiotherapy offer promising outcomes for individuals grappling with balance-related ailments.
Incorporating physical activities and modifications in daily routines emerges as a crucial element in managing balance and spatial orientation disorders. Vestibular physiotherapy utilises specific exercises that stimulate the vestibular system, aiding in its recalibration and subsequently improving symptoms of dizziness, vertigo, and instability.

The therapeutic regimen may encompass balance training, gaze stabilisation exercises, or habituation exercises tailored to an individual’s unique symptomatology. Concurrently, lifestyle modifications such as dietary changes or stress management techniques may bolster treatment efficacy.
This integrative approach not only addresses the physiological aspects but also considers the patient’s holistic needs. It’s paramount for healthcare professionals to promote this innovative method as it fosters self-management while enhancing the overall quality of life for individuals with vestibular disorders.
Transitioning from the multifaceted approach of physical exercises and lifestyle modifications, it becomes crucial to discuss the role of consultation in determining the appropriateness of vestibular physiotherapy.
The individualised nature of this intervention necessitates a comprehensive assessment by a healthcare professional. This involves identifying the specific vestibular disorder, evaluating its severity, and understanding the patient’s overall health status.
The suitability for vestibular physiotherapy is then determined based on these findings. This evaluation also helps customise the treatment plan to align with the patient’s needs.
A rigorous consultation process paves the way for an effective therapeutic strategy that enhances patient outcomes and optimises their quality of life, showcasing how innovation can enhance traditional medical practices like vestibular physiotherapy.