Patellar tendinopathy, also known as jumper’s knee, is a common knee injury affecting athletes and individuals in regular physical activity. It is a condition that involves the degeneration of the patellar tendon, which connects the kneecap to the shinbone.
Patellar tendinopathy, also known as jumper’s knee or patellar tendonitis, is a condition that affects the knee. It is caused by repetitive stress or overuse and is common among sportspeople, particularly those involved in basketball, volleyball, and track and field.
jumper’s knee is a type of knee injury that affects the patellar tendon. This tendon connects the kneecap to the shinbone and straightens the leg. When the tendon becomes inflamed or damaged, it can lead to pain and discomfort.
The symptom is often characterised by pain and stiffness in the knee area. The pain may be worse during activity or after prolonged periods of inactivity. Sometimes, the pain may also be accompanied by swelling or tenderness.
A patellar tendon injury typically causes patellar tendinopathy. This can occur due to a variety of factors, such as repetitive stress and overuse. Athletes who engage in high-impact activities such as running and jumping are particularly susceptible to developing this condition.
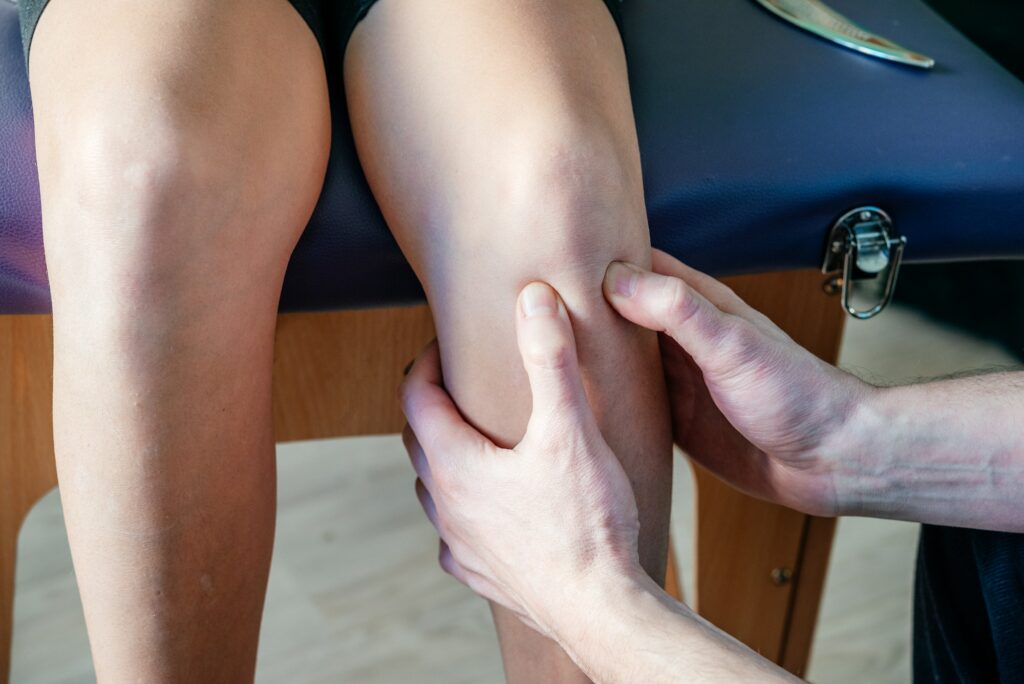
One primary contributing factor to jumper’s knee is the repetitive loading of the patellar tendon. This can lead to microtrauma, which over time can cause the tendon to weaken and become injured. Other factors, such as poor training practises inadequate rest, and muscle imbalances, can also increase the risk of developing this condition.
Repetitive stress is a major contributor to the development of patellar tendinopathy. This is often seen in athletes who perform high-impact activities that place significant stress on the patellar tendon, such as jumping and running. Over time, the repeated force on the tendon can lead to microtears, causing the tendon to become inflamed and painful.
How an athlete trains can also play a role in the development of a jumper’s knee (also see runner’s knee). Overtraining or not allowing enough time for rest and recovery can lead to the accumulation of microtrauma in the tendon. Poor training techniques and incorrect exercise form can also contribute to this condition.

Muscle imbalances can also contribute to patellar tendinopathy. Weakness in the quadriceps and gluteal muscles can increase stress on the patellar tendon. Similarly, tightness in the hip flexors and hamstrings can also increase tension on the tendon, putting an individual at greater risk of developing this condition.
Patellar tendinopathy is typically characterised by knee pain, which can occur during exercise and rest. The pain is usually localised to the patellar tendon, which connects the bottom of the kneecap to the top of the shin bone.
Individuals with patellar tendinopathy may experience stiffness and a reduced range of motion in the knee joint. In some cases, swelling or the appearance of a bump may also occur around the affected area.
As the condition progresses, the pain may become more severe and persistent, making it difficult to perform activities that place stress on the knee, such as running, jumping or squatting.
If you are experiencing any of these symptoms, it is important to seek medical attention to determine whether you have patellar tendinopathy or another knee-related condition.
Diagnosing patellar tendinopathy typically involves a combination of physical examination and imaging techniques. The physical examination will involve evaluating the knee for tenderness, swelling, and range of motion. The doctor may also ask about the individual’s symptoms and medical history.
Imaging techniques such as ultrasound or magnetic resonance imaging (MRI) may be used to confirm the diagnosis and determine the severity of the condition. These tests can identify the presence of tendinosis, which is a characteristic feature of patellar tendinopathy.
Tendinosis can be identified using imaging techniques such as ultrasound or MRI. This condition is characterised by changes to the structure of the tendon, including thickening and disorganisation. It is important to distinguish tendinosis from tendinitis, an acute condition involving the tendon’s inflammation.
Treatment depends on the severity of the condition. In mild cases, conservative treatment approaches usually relieve symptoms and promote healing. Physical therapy and rehabilitation exercises are typically the first step in treatment to strengthen the knee muscles and increase flexibility.
More advanced interventions may be necessary in more severe cases, or for individuals who do not respond to initial conservative treatment. One such intervention is extracorporeal shockwave therapy (ESWT), in which sound waves stimulate healing of the damaged tendon. This treatment has shown promising results but is unsuitable for everyone.
Physical therapy for patellar tendinopathy typically involves exercises focusing on strengthening the knee muscles and reducing stress on the affected tendon. Strengthening exercises for the quadriceps, hamstrings, and calf muscles are essential in reducing strain on the patellar tendon. Additionally, flexibility exercises are important in improving the range of motion and reducing the risk of further injury. Your physical therapist will design a personalised treatment plan based on the severity of your condition and your individual needs.
Rehabilitation exercises are an essential part of treating patellar tendinopathy. These exercises aim to reduce pain and improve mobility. Eccentric exercises, where the muscle lengthens as it contracts, are particularly effective in treating patellar tendinopathy. These exercises typically involve slowly lowering your body weight while bending your knee, such as in a squat. Your physical therapist will guide you through these exercises and monitor your progress to ensure proper form and safety.
In severe cases, more advanced interventions may be necessary. In addition to ESWT, other treatment options include corticosteroid injections, platelet-rich plasma therapy, and surgery. These interventions are typically reserved for cases where conservative approaches have failed or if there is significant damage to the patellar tendon.
Overall, early intervention and a personalised treatment plan are the key to successful treatment of patellar tendinopathy. Working closely with your healthcare team, including your doctor and physical therapist, can help you regain mobility and reduce your risk of future injury.
Dealing with patellar tendinopathy can be challenging, especially for individuals involved in sports or other physical activities. However, several strategies can help you manage this condition and regain mobility.
One of the most important things you can do for patellar tendinopathy is to give your knee time to rest and recover. Avoid activities that cause pain and discomfort, and give your knee the time it needs to heal.
Physical therapy is a key component of patellar tendinopathy treatment. Your physical therapist can create a tailored exercise programme to help improve strength, flexibility, and range of motion. They may also use ice, heat therapy, and massage techniques to reduce pain and inflammation.
Rehabilitation exercises help you regain strength and function in your knee. These exercises typically involve stretching and strengthening exercises, balance training and coordination drills.
If you are dealing with pain and discomfort related to patellar tendinopathy, you can use several pain management strategies. Over-the-counter pain relievers, such as ibuprofen and acetaminophen, can help reduce pain and inflammation. Try topical pain relievers or consult with your doctor about prescription medications.

You should use supportive devices such as knee braces or compression sleeves to help support your knee and reduce the risk of further injury. These can help reduce pain and inflammation and provide additional support during physical activity.
In some cases, lifestyle changes may be necessary to manage patellar tendinopathy. If your condition is related to overuse or repetitive stress, you may need to modify your exercise routine or find alternative activities that put less strain on your knees. Maintaining a healthy weight and eating a balanced diet can also help reduce your risk of knee injuries.
With the right treatment and self-care strategies, it is possible to manage patellar tendinopathy and regain mobility effectively.