Chondromalacia patella might sound like a mouthful, but it’s simpler than you think. It’s a common knee condition where the cartilage on the underside of your kneecap softens and deteriorates. This can cause significant discomfort and mobility issues.
You could be dealing with chondromalacia patella if you’ve been experiencing persistent knee pain, stiffness, or swelling. But what causes this condition? Are there specific risk factors you should be aware of? Furthermore, how is it diagnosed and treated?
It’s heartbreaking to know that simple daily activities like climbing stairs or sitting for long periods can actually cause chondromalacia patella, a painful knee condition.
Patella misalignment is often a major culprit. If your kneecap isn’t tracking properly in its groove, it can lead to excess pressure and subsequent damage to the cartilage.
Sporting injuries are another common cause, especially those involving direct trauma or repetitive stress on the knee joint.
Age-related degeneration naturally plays a part too. As you age, your cartilage may start to wear thin and break down.
Overuse syndromes from high-impact activities like running or jumping may exacerbate this condition.
And don’t discount anatomical variations; if you’re born with an unusual kneecap shape or alignment, it might predispose you towards a chondromalacia patella.
Several risk factors can crank up your chances of developing this nasty kneecap condition.
One such factor is patellar misalignment, where the kneecap doesn’t track properly in its groove causing friction and discomfort.
Repetitive stress injuries from activities such as running or jumping may also increase your risk. Athletes are more prone to developing chondromalacia patella due to their high-demand physical activities.
Gender-based predisposition comes into play too; women are more susceptible because of their wider hips which can cause greater angling of the knees.
Age-related vulnerability also exists: younger people are at higher risk owing to potential growth spurts and unstable knee mechanics.
Knee troubles often creep up stealthily, like a cat on the prowl, initiating their attack with subtle hints such as persistent pain or swelling. You may experience knee instability experiences and joint stiffness factors that hinder your daily activities.

Photo Credit: lovelyday12, Freepik
It’s crucial to recognize these signs:
Ignoring these symptoms could lead to more severe conditions like chondromalacia patella. Therefore, seeking medical advice promptly is essential if you notice any of these signs.
Don’t let your knee troubles get the best of you; a timely medical examination could be a game-changer. Examining joint health is crucial when dealing with symptoms like pain, stiffness, and swelling in your knees.
Diagnostic techniques like X-rays or MRIs can help identify issues like chondromalacia patella.
Your patient history plays an essential role in diagnosis too. Recounting past injuries or activities that might have led to knee problems provides valuable context for your doctor.
Additionally, a physical examination lets your physician assess the extent of damage by checking flexibility, range of motion, and signs of inflammation.
The benefits of early detection cannot be overstated: it’s key to preventing further deterioration and beginning appropriate treatment promptly.
So don’t delay – get checked today!
Getting a glimpse into what’s going on beneath the surface of your skin is possible with imaging tests for knee pain. Radiographic interpretation allows doctors to view images of your knee and spot any signs of chondromalacia patella or other issues that may be causing discomfort.
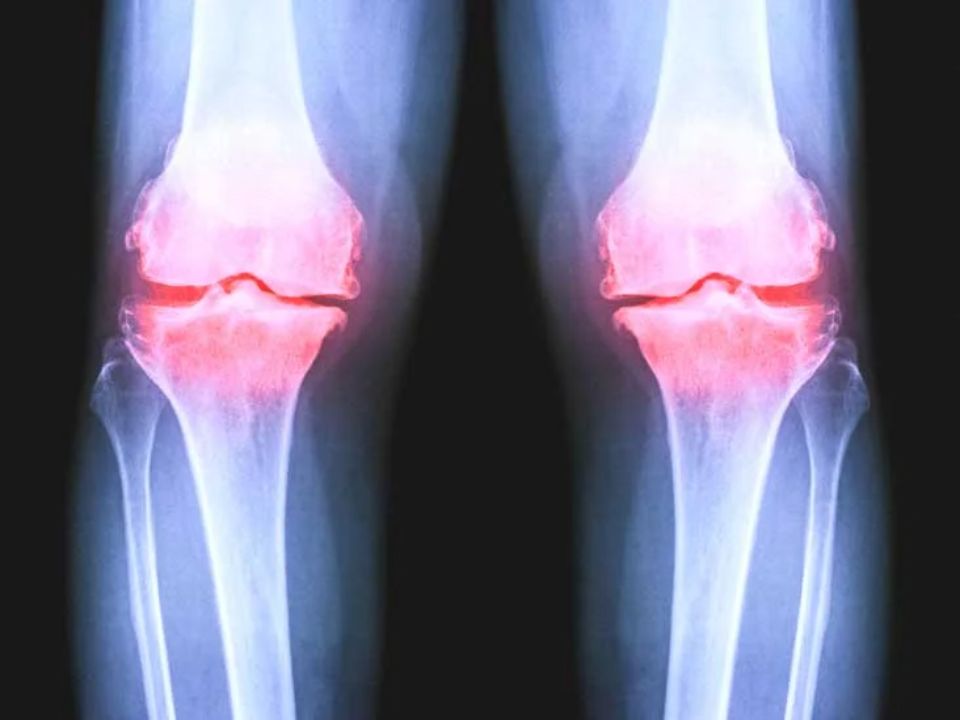
Photo Credit: Healthline
MRI benefits are numerous; they offer detailed pictures of soft tissues, like cartilage and tendons, which X-rays also can’t capture.
Ultrasound advantages include its non-invasiveness and ability to visualize soft tissue structures in real-time.
Contrast arthrography involves injecting dye into the joint to highlight areas of concern on an X-ray.
Meanwhile, Dual energy X-ray absorptiometry measures bone density, which could be reduced if you have long-term chondromalacia patella.
These tests provide valuable insights into your knee health.
Imagine this: you’re finally free from the crippling knee pain, all without having to go under the knife – sound appealing? Let’s explore some non-surgical treatment options for chondromalacia patella.
Remember, it’s important to consult with a healthcare provider before starting any new treatment regimen.
When non-surgical treatments aren’t enough, you might find relief through surgical interventions, which can offer a more permanent solution to your knee pain. Among these options, arthroscopic surgery is commonly used for treating chondromalacia patella. This minimally invasive procedure lets doctors investigate and address the damage inside the knee joint.
Photo Credit: sweet_tomato, Freepik
However, like all surgeries, it’s not without risks. Surgical complications could include infection or blood clots, though these are rare. Once you’ve undergone surgery, post-operative care plays a key role in your recovery speed and overall patient outcomes. Your doctor will guide you through this process, including potential rehabilitation exercises to regain strength and mobility.
Remember that everyone’s experience differs so don’t be disheartened if progress seems slow at times; consistency in following post-op instructions can help ensure an effective recovery process.
You might be surprised at how much power you hold in your own hands to keep knee pain at bay, simply by making some adjustments to your everyday lifestyle.
One of the major exercise benefits is strengthening your leg muscles, which helps support and protect your knees.
Good nutrition impacts joint health positively too, so opt for a diet rich in anti-inflammatory foods like fruits and vegetables.
Weight management also plays a crucial role; shedding extra pounds reduces strain on your knees.
Make regular check-ups part of your routine to catch any potential issues early.
Lastly, don’t underestimate the importance of posture – maintaining correct alignment can prevent unnecessary stress on the knee joints.
Small changes can make a big difference in preventing chondromalacia patella.
With proper treatment, Chondromalacia patella, or runner’s knee, can improve over time. This usually involves rest, physical therapy, and specific exercises to strengthen the muscles around the knee.
While it can be painful and impact daily activities, chondromalacia patella is typically not a serious condition. However, if left untreated, it can lead to more severe knee problems over time.
Surgery is usually considered a last resort for treating chondromalacia patella. Most cases can be effectively managed with conservative treatments such as rest, ice, physical therapy, and non-steroidal anti-inflammatory drugs.
Chondromalacia patella is usually caused by overuse or injury to the knee, such as from running or jumping. Other factors like muscle imbalance or improper knee alignment can also contribute to its development.
Chondromalacia patella is a common condition characterized by the softening and deterioration of the cartilage on the underside of the patella (kneecap). It often causes pain in the front of the knee.
Chondromalacia patella is usually caused by overuse of the knee, improper alignment of the patella, muscle imbalances in the quadriceps, or a traumatic injury to the knee.
The common symptoms of chondromalacia patella include pain in the front of the knee, especially when climbing stairs or after prolonged sitting. There may also be a grinding sensation or a feeling of “giving way” in the knee.
Chondromalacia patella is usually diagnosed through a combination of physical examination, medical history review, and imaging tests such as X-rays, MRI, or arthroscopy to assess the condition of the cartilage and other structures in the knee.
The treatment for chondromalacia patella can vary depending on the severity of the condition. It may include physical therapy, pain management with anti-inflammatory medication, taping or bracing of the knee, and surgery may be needed in severe cases.
The first line of treatment for chondromalacia patella usually involves conservative measures such as physical therapy, strengthening exercises for the quadriceps, and modifying activities to reduce stress on the knee joint.